What is a Cleft lip?
The fourth to seventh weeks of pregnancy are when the lip develops. When the growing facial tissues of an unborn infant don’t completely close, it results in a cleft lip, which is an opening or split in the top lip. A little slit or a wide aperture that extends from the lip into the nose can be present in the lip. A cleft lip can develop on one, both, or even both sides of the lip, as well as very infrequently, in the middle of the lip. A cleft lip and palate can coexist in children.
What is Cleft Palate?
Between the sixth and ninth weeks of pregnancy, the palate (the roof of the mouth) begins to develop. When the tissue doesn’t fuse together when the baby is developing in the womb, it results in an opening or split in the roof of the mouth.
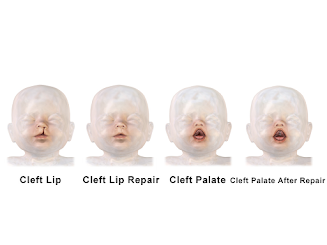
Other Problems: Children with a cleft lip with or without a cleft palate or a cleft palate alone often have problems such as:
- Difficulty with feedings.
- Difficulty swallowing, with the potential for liquids or foods to come out of the nose
- Nasal speaking voice or not able to speak clearly
- Chronic ear infections
- Dental problems.
Ratio: The most prevalent birth malformations are cleft lip and cleft palate. It is generally agreed that one in 1,000 births will result in cleft lip and palate. Nonetheless, socioeconomic status, geographic origin, and ethnic background all significantly impact its occurrence.
Causes and Risk Factors:
Causes:
Most cases of cleft lip and cleft palate are caused by an interaction of genetic and environmental factors. In many babies, a definite cause isn’t discovered.
Risk Factors: There are a number of risk factors that can raise a baby’s chance of having cleft lip and cleft palate, including
- Family History: Having a child with cleft lip or palate is more likely for parents who have a history of the condition.
- Diabetes: Compared to women who did not have diabetes, women who were diagnosed with the disease prior to becoming pregnant had an increased risk of having a child with a cleft palate.
- The use of specific medications increases the chance of birth abnormalities, such as cleft lips and palates. These medications are prescribed to treat or prevent seizures.
- Smoking or Alcohol: Women who smoke or drink alcohol are more likely to have a baby with cleft compared to women who do not smoke or drink alcohol.
When to see a doctor?
A cleft lip and cleft palate are usually noticed at birth, and your doctor may start coordinating care at that time. To correct the condition, you will likely work with a team involving a plastic surgeon, maxillofacial surgeon, otolaryngologist (ear, nose, and throat specialist), general dentist, orthodontist, and oral surgeon.
For more information visit Best Dental Clinic in Ahmedabad- Teeth Care Centre Dental Hospital

